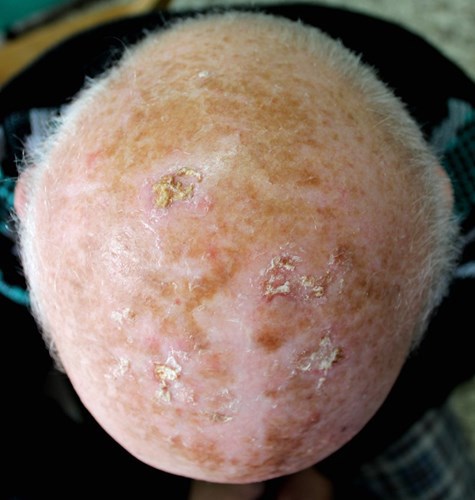
Photodynamic therapy (PDT) is a non-surgical treatment which uses a light-sensitive drug (photosensitizer) to destroy cancer cells. It can be used to treat different types of cancer, including a type of skin cancer called basal cell carcinoma (BCC).

With PDT, the cancer cells absorb more of the photosensitizer over time than normal tissue. After this, a bright light is shone on the affected area to cause a reaction to kill the cancer cells.
At The Christie in Manchester, PDT is used as a treatment in the PDT clinic to treat BCCs. If you have a BCC or multiple BCCs, your consultant will discuss with you whether PDT is right for you.
We can also use daylight PDT to treat a condition called actinic keratosis. Actinic keratosis causes scaly patches of skin. It is generally caused by sun exposure over several years. Actinic keratosis isn’t cancer but there is a chance that it could become cancerous if it isn’t treated. Daylight PDT works in a similar way to traditional PDT but it uses the sun's rays as treatment.
Treating basal cell carcinomas with photodynamic therapy
Basal cell carcinomas (BCC) respond very well to treatment with photodynamic therapy (PDT). If they are not too deep (around 2mm), they usually have excellent cosmetic results.
More than one BCC can be treated simultaneously in a single treatment session, and the treatment can be repeated if required.
- First, you will have any loose dead skin cells removed using fine dermatological paper or a curette. Then, you may need an ultrasound scan to accurately determine the depth of the BCC.
- Next, you will have a cream applied directly on to the lesion using a spatula. You may feel a slight stinging when the cream is applied.
- You will then have a dressing applied over the lesion. The dressing will be kept on for 3 hours to enable the photosensitizer to be absorbed by the lesion. You can leave the building during this time, but you should keep the dressing on and return for your appointment approximately 3 hours later.
- Next, your dressing will be removed. The lesion will be examined using low levels of UV light to determine the uptake of the drug and the lesion will be outlined. You may have a local anaesthetic at this stage. You might also have a mask applied to your skin to shadow the areas of healthy tissue next to the BCC from the PDT light.
- You will then sit or lie down in a comfortable position. A lamp containing bright red light emitting diodes (LEDs) is placed approximately 8cm away to illuminate the lesion. Additional cooling fans will be used to minimise and stinging sensations. This light isn’t a laser, but it may be uncomfortable to view. You may be offered goggles to shade your eyes depending on the location of your BCC.
- The lamp is then switched on and set to deliver a fixed dose of red light to your BCC. You may experience a slight stinging or prickling sensation at this stage although the use of a local anaesthetic and cooling fans will help to minimise this. The lamp will illuminate the BCC for between 8 to 25 minutes dependent on the treatment. During this time, you will need to keep still. The treatment can be paused at any time if you need to move urgently.
- After the lamp has delivered the required dose, you will have a dressing applied to the area. You will need to keep this dressing in place for 2 days after the treatment to keep light away from the area.

Post-treatment after your photodynamic therapy
You can apply a mild topical steroid after your photodynamic therapy (PDT) to aid with any swelling in addition. You will also need to keep the area covered for 2 days following treatment.
You can use simple moisturisers such as petroleum jelly to soften crusts and reduce itch following the initial 2-day period. This will need adjusting according to our current advice.